Pearls of Knowledge: Reentry

Interpreting Rhythms: Reentry
Pearls of Knowledge © BrainyNurses.com
Reentry is one of the most common causes of supraventricular and ventricular rhythms. It is seen with atrial fibrillation, atrial flutter, and runs of beats such as in ventricular tachycardia or paroxysmal atrial tachycardia.
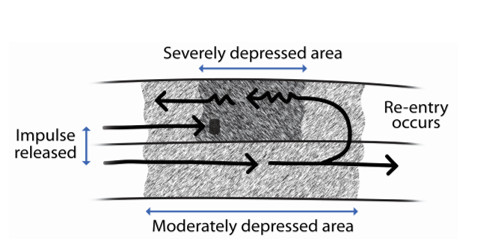
Typically, the myocardial tissue is depolarized and then becomes refractory. In patients with structural heart disease, or scar tissue from ischemia or infarction, a change in conduction occurs in some of the myocardial tissue and the tissue is not depolarized at the same time. Reentry occurs when a portion of the tissue is reactivated by an impulse that had already stimulated it.
Local reentry
Local reentry occurs within a small area (single site) of the atrium or ventricle such as atrial flutter, ventricular tachycardia, or paroxysmal atrial tachycardia. In atrial fibrillation, multiple reentry circuits are present resulting in the chaotic P waves.
Atrial flutter
(Most often occurs at atrial rates of 300 BPM but can range from 250-450 BPM.)

Ventricular tachycardia
(Heart rate generally between 140-200 BPM.)

Paroxysmal atrial tachycardia
(Heart rate generally between 120-250 BPM.)

Atrial fibrillation
(Ventricular rate varies depending on the degree of AV block.)

Global reentry
Global reentry involves activation of the entire conduction system and is seen in Wolff-Parkinson-White (WPW). In WPW, there are one or more accessory pathways. When an impulse occurs, it enters the ventricles by going through the AV node and the accessory pathway. This results in a short PR interval, a delta wave (slurring of the QRS), and a wider QRS complex.

When an early beat occurs, the “normal” conduction is refractory and allows the impulse to go up or down just the pathway and results in a tachycardia. Typically, it is a narrow complex. When it is a wide complex, it resembles ventricular tachycardia, and is more dangerous.
WPW in sinus rhythm (Short PR, delta wave, and wide QRS)

WPW in reentry (and resultant narrow complex tachycardia)


